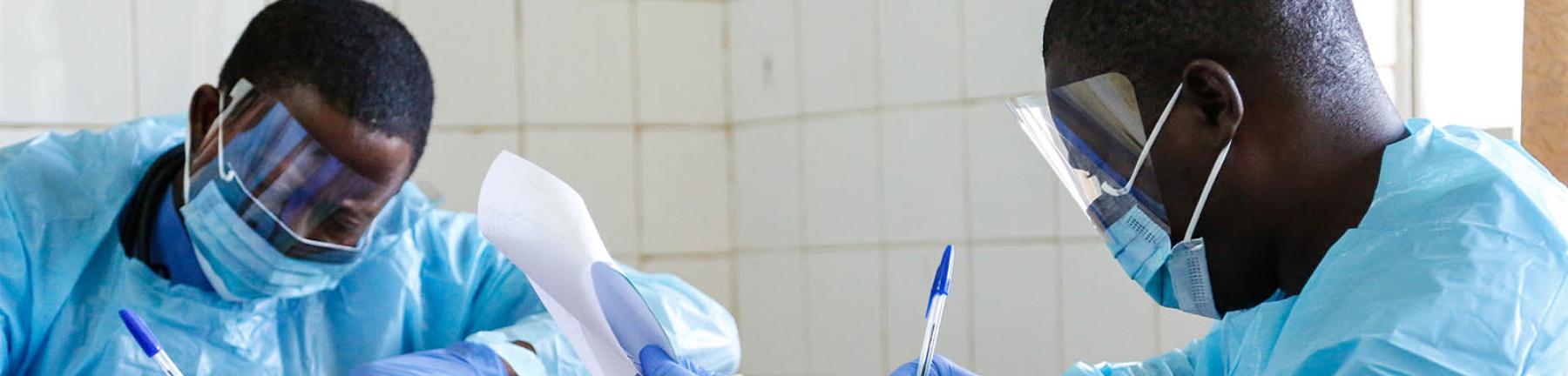
How can global health systems be strengthened to respond to shocks like Covid-19?
Research from our Maintains programme in Bangladesh, Pakistan, Uganda, Kenya, Ethiopia and Sierra Leone during Covid-19 considers the links between health system strenthening and shock responsiveness.
-
Date
January 2021
-
Areas of expertiseClimate, Energy, and Nature , Health
-
FeedWEF
-
KeywordsDisaster risk , Shock response , Health monitoring, evaluation, research, and learning (Heath MERL) , Community health workers (CHWs) , Covid-19 , Universal Health Coverage (UHC)
Now more than ever, strong, equitable health systems are vital. The global pandemic has shown the crucial need for health security with Covid-19 highlighting gaps in the systems needed to prevent and control disease outbreaks – such as surveillance, testing, and quarantine. Alongside these more specialist capacities, experience from past epidemics shows the importance of robust underlying health systems for an effective response to emergencies. Countries need functional health system ‘hardware’, such as adequate health workers and funding, and ‘software’, including coordination mechanisms and community trust in the health system. This underlying health system capacity enables both effective response to the crisis, and continuity of essential services such as antenatal care in the face of increased or changing demands. The importance of strong underlying health systems has been emphasised in relation to Covid-19 by global actors such as the World Bank, WHO, and Universal Health Coverage (UHC) partnership among others.
However, as these stakeholders suggest, strong basic health systems alone are not enough, and countries also need specific public health and health security capacities to deal with outbreaks or other shocks. Strengthening emergency preparedness needs combined investment in both strong health systems and primary health care, and emergency management.
Research shows the role of health system strengthening and emergency preparedness
Research from our Maintains programme has shown the importance of both underlying health system capacities and emergency-related systems. Community health workers (CHW) are widely recognised as playing valuable roles for health service access, and investment in CHW is often part of strategies for strengthening health systems. In several countries, CHW have played important roles in the response to Covid-19. For example, CHW in Sierra Leone undertook contact tracing and community engagement, and in Bangladesh, CHWs have helped with case identification and monitoring home quarantine. In India and Ethiopia, networks of community health workers have played critical roles in community education, screening, and case identification.
The pandemic has also highlighted the need for further support to CHW and strengthening of the human resource base. In Sierra Leone, diversion of CHW to Covid-19 activities took their time from other important services, and wider staff shortages hindered the response. Many low-income countries had insufficient health workers before Covid-19, making it particularly difficult to balance the demands of responding to the pandemic alongside maintaining other essential services. Governments have tried to rapidly boost the health workforce, for example through rapid recruitment in Bangladesh, Pakistan, and Uganda, as well as cancelling leave or mobilising retired professionals in some countries.
The Covid-19 experience also shows the importance of specialist emergency functions in the countries where Maintains operates. Bangladesh, Pakistan, Kenya, Uganda, Ethiopia, and Sierra Leone have all been active in implementing strategies such as testing, contact tracing, quarantine, and community education. Past investment has enabled response: in Sierra Leone, the experience of previous shocks such as Ebola contributed to investment in surveillance and reporting structures that could be activated for Covid-19. These systems require further investment to overcome challenges such as continued paper-based reporting in some frontline facilities, and to enable prompt data.
Beyond Covid-19, our research on other shocks has also shown the need for both health system strengthening and specialist emergency capacity. In Kenya, health system and emergency response capabilities have been strengthened considerably over the past decade. However, in the north of Kenya, the health system has little spare capacity (including staff and finance) to cope with spikes in malnutrition and disease caseloads associated with drought. This leads to heavy workloads and stress for staff. Alongside basic health systems investment, the research found areas to strengthen in shock-related systems. In particular, health and nutrition are not yet fully integrated within drought management arrangements, including the early warning system and contingency funding. Consequently, the health system remains largely dependent on international aid to address major surges in demand, especially for providing nutrition products and integrated outreach services for remote communities in the arid and semiarid lands.
Promoting equity and addressing the social determinants of health
Investment in UHC and emergency preparedness must address equity and inclusion. Equity is at the core of UHC, with a focus on ensuring everyone can access good quality care without financial hardship. Covid-19 has been widely recognised as exacerbating inequalities, in health and more broadly. Gender is an important divide. Women have faced constraints in access to services such as antenatal care, labour market insecurity, increased caregiver responsibilities and risks of gender-based violence. Health workers are often female, particularly at community level. Covid-19 has brought risks for their physical and mental health, with inadequate protective equipment, difficulty in balancing professional demands, and increased household care.
Socioeconomic divides have also been stark. For example, inadequate access to clean water is a long-standing challenge for many communities in low-income countries, highlighted by Covid-19. In Sierra Leone, many households lack easy access to water, limiting their ability to comply with lockdown measures. Lack of water in health facilities and quarantine centres was also a concern, hindering implementation of infection prevention and control measures. Clean water supplies have been a particular challenge in refugee camps, for example in Bangladesh. Income and livelihood strategies have also heightened risks of infection and ability to follow control measures for some groups, for example through employment that requires repeated interactions and reliance on daily income. Precarious economic situations also create other health risks. In Ethiopia, public health control measures limited employment for groups such as day labourers and restaurant staff, and falls in income combined with higher food prices increased food insecurity. This influence of the social determinants of health highlights the need for investment in sectors beyond health to enable response and support positive health outcomes.
What will our research bring?
Over the next two years, Maintains research will consider these interactions between health systems, emergency preparedness, equity, and the social determinants of health. Our conceptual framework for shock responsive health systems (version 1 here, a second version will be published soon) highlights the role of basic health system hardware and software, as well as the influence of connected systems such as water and social protection, and the important influence of inequalities in health service access and outcomes. Country studies will examine ways that different health system components enable or hinder emergency response, and capacities required for countries to implement effective strategies for shock prevention, preparedness and response. We will also look at links between health system strengthening and shock responsiveness. For example, research with government partners in Ethiopia will consider how a health system strengthening investment designed to improve the quality of community and primary care contributes to shock preparedness and response, and what additional support is needed to ensure resilience. We will continue to share findings on the Maintains website.
Authors: Kate Gooding, Alhassan Kanu, Matt Fortnam, Debbie Hillier
For more information on this programme contact: [email protected]
This blog was originally published on the Maintains website in December 2020.
Photo credit: FCDO/ Simon Davis: Doctors working at Connaught Hospital, Freetown, Sierra Leone