Meet the challenges: Rolling out Covid-19 vaccination in low-and middle-income countries
What are the barriers to Covid-19 vaccine distribution and how can countries potentially minimise these challenges?
-
Date
February 2021
-
Area of expertiseHealth
-
FeedWEF
-
KeywordHealth service organisation and delivery (HSOD)
The world has witnessed an unprecedented race to develop efficacious vaccines to stop the devastating consequences of the Covid-19 pandemic. By mid-January 2021, there were nine vaccines approved to be used in different countries. Now, as some countries have started to mass-vaccinate, we have considered some of the challenges that low-and middle-income countries (LMIC) may face and how these challenges may potentially be mitigated (Figure 1).
Figure 1 Possible bottlenecks for successful roll out of Covid-19 vaccinations in LMICs
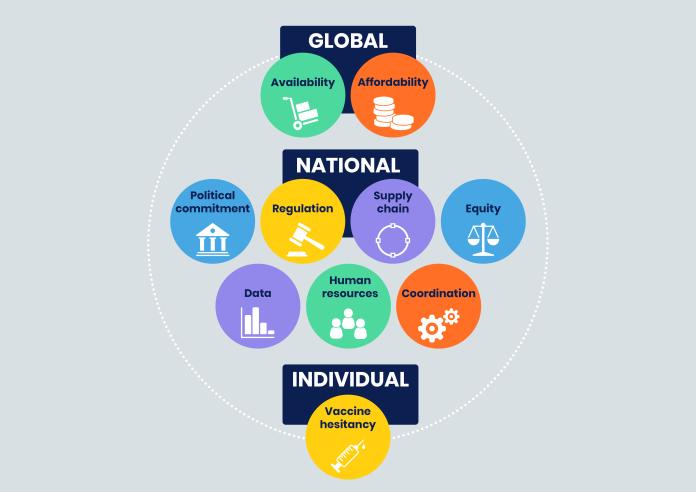
Global level
Availability: One of the most critical challenges for LMICs currently is to get sufficient supplies of vaccine and to sustain the level of supplies needed. In September last year, Oxfam reported that the richer nations -with just 13% of the world’s population - secured more than half of the supplies of the five leading vaccine candidates at that time. The COVID-19 Vaccine Global Access Facility (COVAX) has been established to ensure rapid, fair and equitable distribution of the vaccine across the globe. The success of COVAX will be a key determinant for ensuring availability of vaccines in LMICs with 67 low income countries relying on COVAX for their vaccine supplies.
Affordability: The price of vaccines will certainly be a major factor in countries’ ability to roll out mass vaccination. Prices of the approved vaccines vary widely, reported as ranging from USD 6 to USD 74 per dose. COVAX alone will not be able to meet the demand of LMICs for COVID-19 vaccines and countries’ ability and affordability to secure additional vaccine, possibility at a higher cost, will be critical for vaccine roll-out, especially at the early stage.
National level
Political commitment: Strong political commitment is crucial for the success of a massive initiative such as the roll-out of Covid-19 vaccines. A recent panel discussion of members of parliaments from several countries, including LMICs, led by Lord Boateng of the UK Parliament identified cross-party, financial, legal, civil-society and grassroots commitments as the cornerstones for success of national immunization. These domestic political commitments are equally, if not more, important for Covid-19 vaccination.
Regulation: Even if countries can secure their fair share of vaccine, national regulatory approval is needed before administration. While the drug administration authorities in high income countries are generally well equipped to rapidly review and approve vaccines that are successful in clinical trials, nearly three-quarters of national regulatory authorities worldwide lack the capacity to do so. Thankfully, LMICs can use WHO’s Emergency Use Listing (EUL) process for emergency approval within their countries for the vaccines that are listed in EUL.
Supply chain: Many LMICs lack the supply chain infrastructures to store, transport and deliver vaccines effectively. This is particularly important for the requirement of maintaining cold chain ranging from 2°C to -80°C and will contribute to determining which vaccine it is feasible to distribute in each country as the vaccines have differing cold chain requirements. In addition to the difficulty of maintaining cold chain, limitations of storage space, lack of transportation, hot and wet tropical weather create additional challenges for many LMICs. Careful piloting can help ensure that the entire supply chain can run smoothly without jeopardising other activities such as routine immunisations for children.
Equity:. Ensuring equitable distribution of the vaccine to the population most at risk is a critical and substantial challenge for many countries. Various targeting strategies are being adopted to determine the domestic allocation by countries. However, without careful attention these strategies have the risks of being inconsistent, not evidence based, and most importantly lacking equity. To ensure equity countries need to follow evidence based targeting strategies based on three key ethical principles: preventing harm, prioritizing the disadvantaged and achieving equal treatment.
Data: Identifying the priority populations and vaccinating them is not as straightforward in LMICs as it is in many high income countries due to a lack of centralised data to identify those most at risk. Whilst it may be possible to identify priority groups such as healthcare workers and elderly people, identifying people with underlying medical conditions (e.g. diabetes, heart diseases etc.) is more difficult. These data gaps have been identified as limitations for estimating targets for Covid-19. Countries may consider registering people with underlying medical conditions using mobile technologies with verification while the vaccine is being procured, shipped and the essential workers and the elderly are being vaccinated.
Human resources: Health worker density is significantly associated with the coverage of routine vaccinations. A skilled workforce required to implement a vast endeavour like Covid-19 mass vaccination is likely to be a major bottleneck in many LMICs. To supplement these human resources, the countries may consider engaging the Non-Governmental Organization (NGO) sector which has proven success in delivering many initiatives in many developing countries. Some counties may also consider involving defence forces.
Coordination: The Covid-19 response involves multiple stakeholders including health department, local government department, civil society, development partners, private sector, community members etc. Therefore, in addition to the organisational and logistical measures to roll-out a mass vaccination programme, countries need effective governance. Effective coordination between multiple stakeholders is a significant challenge. However, many LMICs have practical experience in coordinating humanitarian response and the success of implementing mass Covid-19 vaccination may largely depend on the level to which they can leverage that experience.
Individual level
Vaccine hesitancy: Covid-19 vaccination hesitancy is strong and widespread in many parts of the world. Thankfully, prior evidences suggests that in LMICs vaccine coverage is mainly correlated with supply side factors such as vaccine availability, whereas in high income countries it is more correlated with personal belief. However, increasing rumours linked to social and digital media are leading to growing mistrust of vaccines and vaccine trials in LMICs. Effective and targeted community engagement and communication campaigns can help in mitigating vaccine hesitancy in countries where the risk is substantial.
The challenges mentioned above are not exhaustive, nor are the mitigation measures suggested complete or guarantors of success. The aim of this article is to highlight some of the issues and potentially to function as a checklist for decision-makers while rolling out COVID-19 vaccinations in LMICs. While vaccination is the most promising “way out” from this pandemic, it will take months if not years to have a substantial population of LMICs being vaccinated in order to have an impact. In the meantime, the countries will have to juggle with various strategies in order to control the virus.

