Climate Finance for Powering Healthcare
Addressing the urgent need to 'climate proof' healthcare facilities across South Asia and Sub-Saharan Africa.
Project team members
Elizabeth Gogoi , Saumya Vaish , Kenneth C. Ene , Apar Paudyal , Shamim Zakaria
-
DateAugust 2023 - December 2023
-
Client
SEforAll
-
Project number
A6509
-
Project status
Active
Nearly 1 billion people in low- and lower-middle-income countries are served by healthcare facilities without reliable electricity access or with no electricity access at all. Many are using fossil fuels to supplement grid-supplied electricity, such as diesel generators and kerosene lamps. This is causing indoor air pollution and contributing to greenhouse (GHG) emissions. Healthcare facilities across South Asia and Sub-Saharan Africa are also vulnerable to climate impacts, such as extreme weather events. There is an urgent need to ‘climate-proof’ such facilities: To provide a secure supply of clean energy, reduce the facilities’ energy and carbon footprint and build their resilience to climate impacts. We carried out a study on the potential of climate finance to support the uptake and scaling of low-carbon and resilient solutions for health-care facilities in South Asia and Sub-Saharan Africa.
Overview
The global healthcare sector had a climate footprint of 2GtCO2e in 2014, equivalent to 514 coal-fired power plants. There is no accurate carbon footprint for healthcare facilities in South Asia and Sub-Saharan Africa, although the healthcare sector as a whole represents an estimated 4 percent of national emissions in these regions. However, most public sector healthcare facilities are not consuming energy at the level required to deliver high-quality health services, due to the unreliability and costs of electricity and the availability of doctors and other ‘demand’ issues.
To achieve better healthcare outcomes, facilities in South Asia and Sub-Saharan Africa will on average need to consume greater volumes of energy in the future. The source of the energy used to power healthcare facilities today and in the future influences their carbon footprint. Currently, a significant proportion of facilities are supplementing with grid-supplied power with generators that use fossil fuels and emit considerable health-affecting air pollutants.
Healthcare facilities in these regions are already being affected by climate change, particularly extreme weather events which are expected to worsen in the future. For example, devastating floods in Pakistan in 2022 damaged 10 per cent of all healthcare facilities, leaving 8 million people without access to urgent health services.
Challenges
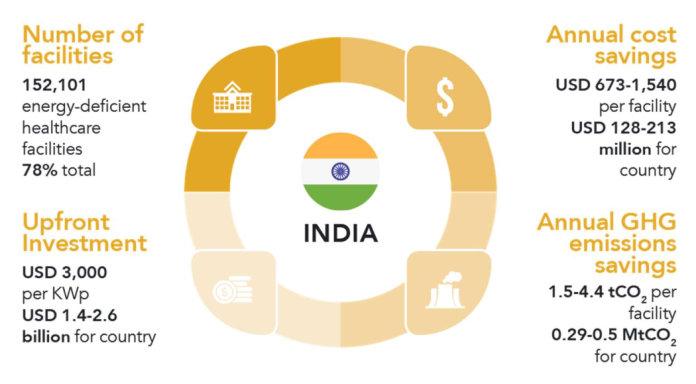
We supported Sustainable Energy for All (SEforAll) to explore the potential of climate finance to support healthcare facilities in South Asia and Sub-Saharan Africa to adopt low-carbon and resilience-building ‘solutions’. This includes technologies, measures and approaches that are viable and available but due to various financial and other barriers are not widely used. For example, we estimated that if a healthcare facility installed a stand-alone solar system they would save approximately 1.4- 4.2 tonnes CO2e every year from the use of fossil fuel generators and would be more resilient to a disruption to the electricity grid in case of a storm or other hazard. The facility would also save approximately USD 630 – 1,411 every year from fuel savings. The figures below show what impact this would have if all energy-deficient facilities in India, Nigeria and Nepal adopted solar systems.
 |
 |
 |
To get this and other climate solutions adopted by a large number of healthcare facilities in South Asia and Sub-Saharan Africa there are various costs that need to be considered. This includes the upfront cost of any capital, ongoing maintenance and operation costs but also investments needed to strengthen the policy, regulatory and institutional system that would support the adoption of such measures at scale. We studied five sources of climate finance – bilateral climate finance, multilateral climate funds, private foundations, carbon and renewable energy markets and green bonds – to see whether and how they could cover such costs.
Expertise
Each of the sources of climate finance has its own mandate, access requirements and delivery modalities. We used our own and others’ experiences of supporting governments to access climate finance to identify how non-government partners, such as SEforAll, can support governments in South Asia and Sub-Saharan Africa to use the financing available to climate proof their health-care facilities. Non-government partners role ranges from playing a supportive and influencing role (for most bilateral funds and green bonds) to directly designing and mobilising funds (for some multilateral funds, private foundations and carbon markets).
We identified a set of barriers to using climate finance for climate-proofing health-care facilities and specific actions that non-government partners can take to address these issues. For example, the potential GHG emissions savings that can be expected from a single facility adopting low-carbon measures such as a solar system is too small to attract climate finance by itself. Therefore, aggregating a large number of facilities under a programmatic approach will reduce the transaction costs and make it more viable for climate finance. To facilitate access multilateral funds such as the Green Climate Fund a project can be designed to deliver both mitigation and adaptation benefits thereby increasing the expected impact or returns of the funds’ investment.
Impact
Our analysis highlighted five key priorities to help mobilise climate finance for low-carbon and climate resilient measures for healthcare facilities:
-
Do an accurate assessment of local facilities’ energy, climate and health needs - for today and in the future – to identify costs and benefits of investments in climate-proofing.
-
Prepare a long-term facility-level and national financing plan - for both the upfront capital costs but also the recurrent operation and maintenance costs – to identify the most appropriate source of climate and non-climate finance.
-
Breakdown silos between healthcare sector professionals and experts in energy and climate finance.
-
Design a programme involving a large number of facilities to deliver economies of scale but which also strengthens the wider enabling environment to encourage the further scaling out of the climate solutions.
-
Prioritise the digitalization of healthcare facilities – including monitoring emissions and energy consumption – as a prerequisite for any climate finance source.
Non-government partners such as SEforAll can play an important role in attracting climate finance for healthcare facilities. This includes raising awareness and increasing demand for climate finance among national healthcare sector stakeholders. They can also play a convening role bringing together experts in health, climate and finance (who typically do not work together) to co-design a strategy and specific programme that targets climate finance.
